Fort Worth Medical Students Connect Basic Sciences and Clinical Skills in Team-Based Learning Environment
Second-Year Medical Students at TCU and UNTHSC School of Medicine begin Phase 2 with 40 Learning and Pondering Sessions (LeAPS).
FORT WORTH – For their first in-person class since the beginning of the COVID-19 pandemic, second-year medical students saw human anatomy from a whole new perspective.
“The technology is amazing,” said Ruthvik Allala, a second-year medical student at the TCU and UNTHSC School of Medicine. “With cadavers you have a lot of variability in between because it’s different bodies. With the HoloLens you see a textbook version of what you would see if there was a perfect anatomical representation of something. It makes it easier to understand within a broad scope. Having the chance to do both is going to be great for medical students going forward.”
It was a three-dimensional perspective of every part of the human body to be exact using the Microsoft HoloLens™ and the HoloAnatomy™ Software Suite developed by Case Western Reserve University.
The experience was the first of 40 Learning and Pondering Sessions (LeAPS) during Phase 2 of medical school.
In LeAPS, the 60 medical students are put into small groups once every week where they can focus on connections between the basic sciences and clinical sciences in a supportive team-based learning environment.
“They are learning about their Longitudinal Integrated Clerkship (LIC) curriculum as well as spiraling in basic science from the first year,” said Whitney LeFevre, M.D., assistant professor at TCU and UNTHSC School of Medicine.
The first LeAPS was titled, “When One Patient Becomes Two,” and was centered around pregnancy and the newborn baby.
The students rotated through four hour-long sessions where they took part in interactive discussions about getting pregnant and the first trimester; simulation of a female patient in active labor; a postpartum visit with a mother and child; and a newborn baby experiencing problems post-delivery.
“I think our students are really lucky that they get clinical learning a few days each week from day one,” Dr. LeFevre said. “Now in Phase 2, we’ve sort of flipped that and they are in the clinical learning environment most of the time and we only have them one half day” where we can combine all of the learning.
Module 1: Getting Pregnant and The First Trimester
The medical students were presented with three different cases: a female patient and her spouse who have hopes of conceiving a child; a pregnant patient who is no longer with her spouse; and a follow-up visit after counseling.
“It helps them (medical students) understand that having a healthy mom helps you have a healthy baby,” Dr. Lefevre said.
The students discussed counseling, which is often referred to as preconception care. The goal is to optimize, whenever possible, a woman’s health and knowledge before planning and conceiving a pregnancy in order to eliminate, or at least reduce, the risk associated with pregnancy for the woman and her future baby.
On the flip side, if pregnancy is not desired during this type of counseling, the students learned how current contraceptive use and options can be discussed to assist the patient in identifying the most appropriate method for her and to reduce the potential for an unplanned pregnancy.
The session also covered difficult counseling topics, like discussing abortion options if the patient is experiencing pregnancy issues or complications.
“What that really tells us is that there are other factors that really play into a patient’s decision or the way they decide to do something,” said Kavneet Kaur, a second-year medical student at the Fort Worth M.D. School. “Our role as a medical provider is to be there for them and to support them and also find out what those factors are so we can get them the appropriate resources.”
Module 2: Simulation of a Female Patient in Active Labor
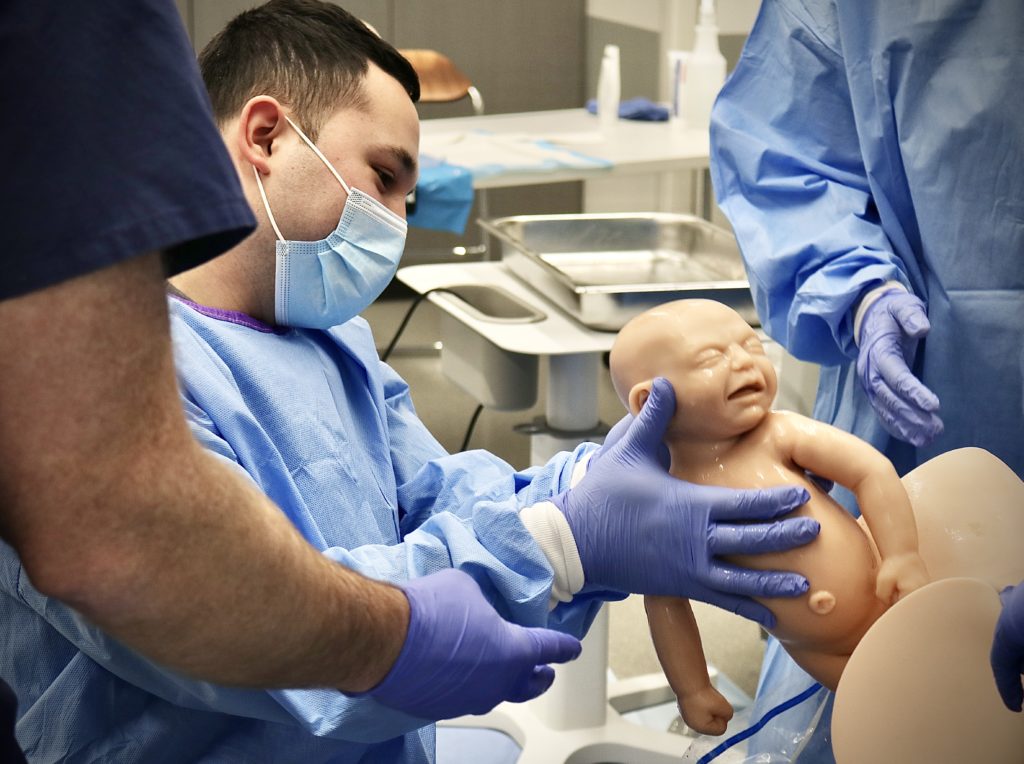
The joy of experiencing childbirth and delivering a baby for the first time is something most medical students never forget. For Kaur, she had gone through that experience one day earlier at her LIC.
“The great thing about LIC and being in clinic from day one is that I go to my LIC and I see a patient and I see a baby delivery,” Kaur said. “Then, I come in the next day and I do my LeAPS and we have a simulation of pregnancy and a delivery so I can relate easily.”
For the first portion of the simulation, the students were put into groups of three to four and each student was assigned a role: resident, attending or nurse.
The simulated female patient was 25 years-old and an A1 diabetic presenting in active labor. Her labor progress has been slow and she’s on Pitocin for labor augmentation. She also developed a fever an hour earlier and was given antibiotics. The woman has been pushing for two hours and now the baby’s head is finally crowning.
“As this is happening I’m relating what I did in my LIC and in my OB-GYN rotation,” Kaur said. “I know what I’m supposed to do. I know what I’m supposed to say to the patient. I know what it feels like so I’m more comfortable.”
The students also switched roles and went through a simulation where their team prepared the resuscitation table for a newborn after delivery. They also went over basic Neonatal Resuscitation Program (NRP) steps to take if a baby has poor tone and is not breathing or crying at birth.
At the end of each session, the students debriefed with their classroom instructors to fill in gaps on both cases, answer questions and practice anything they wanted to practice again.
“They are seeing this stuff in clinic and they are starting to bring that into the conversations,” Dr. LeFevre said. “It’s great to see them start to put pieces together of things that they’ve experienced into the clinical learning here on campus.”
Module 3: The 4th Trimester and HoloAnatomy
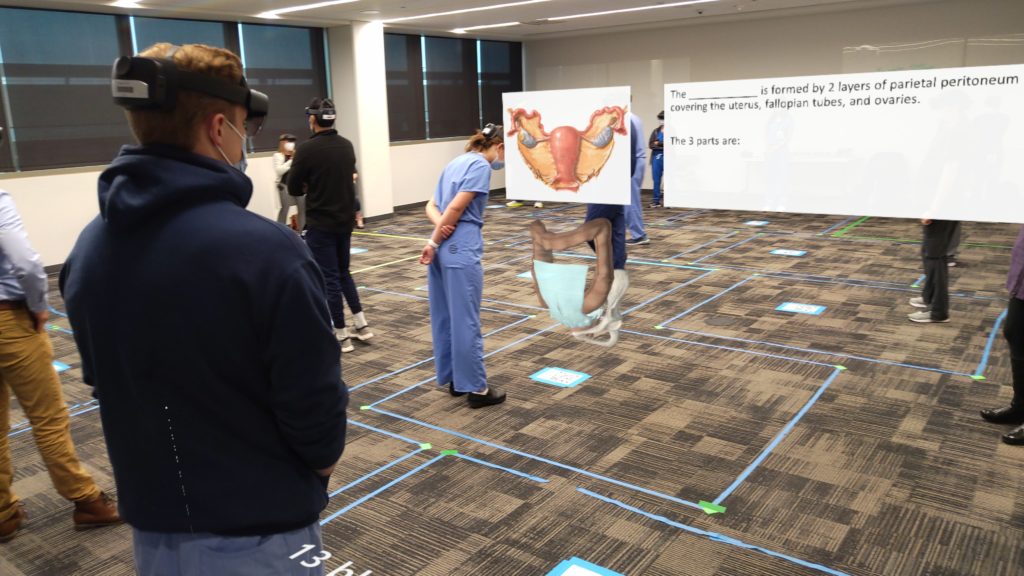
For the third session, the medical students put themselves in the role of a primary care physician.
The first half of this session focused on a two-week postpartum visit. The students were the primary care doctor for the mom and the baby and had even been present for the child birth. As the students prepped themselves to have a conversation with the mom, Dr. LeFevre wanted them to keep some points in mind for the visit: the main components of the postpartum visit; understanding the Phq9 and Edinberg Depression Scales, taking care of mom is taking care of the baby; and lactation resources for mom if she hasn’t been able to breastfeed.
“It’s sort of relating OB-GYN and pediatrics and family medicine that they are all doing weekly,” said Dr. LeFevre. “Seeing how they all kind of connect and integrate.”
The second half of the session used the Microsoft HoloLens ™ and HoloAnatomy™ to review some basic pelvic anatomy with the medical students. During the exercise, the students were asked to describe the blood supply to the uterus, tubes and ovaries, describe the course of the ureter from kidney to the bladder in the female pelvis and identify common landmarks during pelvic surgery to avoid that can lead to bleeding and urinary tract complications.
Seeing the anatomy come to life right in front of the students using the HoloLens is quite different from how anatomy is taught at other medical schools, according to Dr. LeFevre.
“It’s really cool how they can see the three-dimensional reality,” said Dr. Lefevre. “I learned anatomy on a cadaver in my first year of medical school and I never went back to it and then I was expected as a clinical student to know everything in a three-dimensional way.
One way to describe using HoloLens and HoloAnatomy together is like having images from a textbook jump off the page and give you the ability to look inside and around every layer of the anatomy in a real-world environment, according to second-year medical student Allala.
“You put it on and it’s pretty intuitive,” Allala said. “I’m excited for the future of it and I’m excited for our MS-1s (first-year medical students) because they are learning a lot of their anatomy through it and it should pay dividends for them and us and really push our anatomy knowledge pretty far along.”
Module 4: Newborn Exam and Respiratory Distress of the Newborn
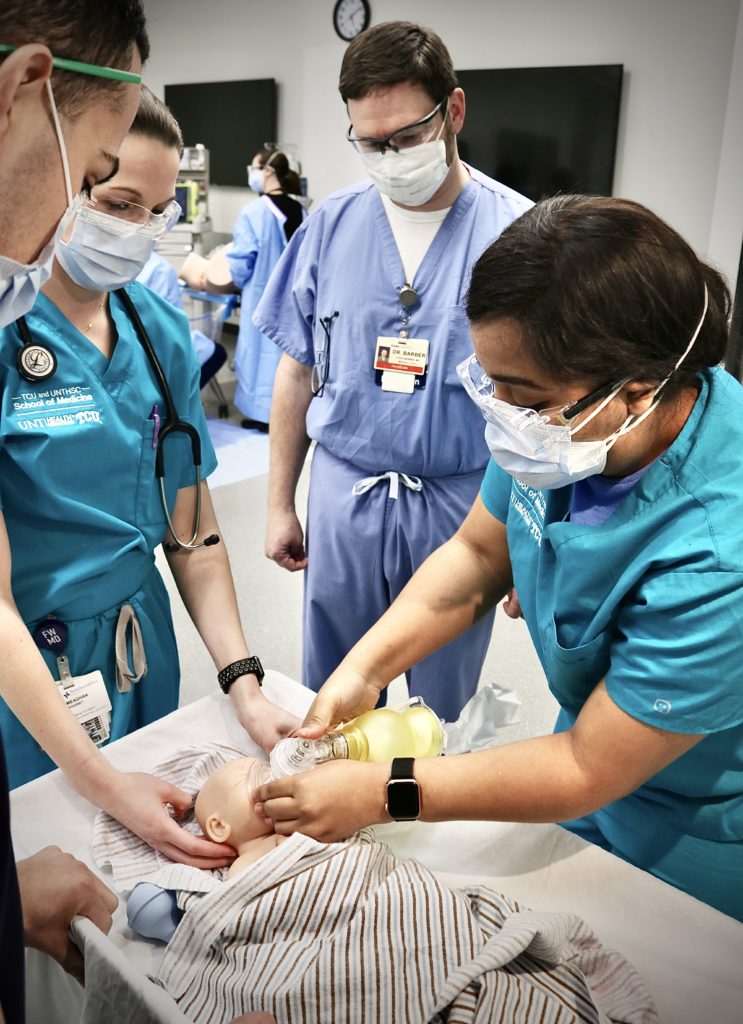
For their final session, the medical students were introduced to a manikin of a 37-week newborn child.
While in the nursery, the baby developed respiratory issues two hours post delivery. The students were put into groups that performed the steps of a newborn exam.
“As a baby is born and as they grow physiologically they’re having changes that are happening to them as they develop,” Kaur said. “Being able to understand the differences from when they are one-month-old to three-months-old and the different reflexes they should be having and those small details from the developmental milestones that’s what we were trying to get.”
They also had to learn to identify signs of distress in a newborn to wrap up their session.
“All of these LeAPS are just a great way for them to start pulling those pieces together and seeing how we think about patients clinically,” Dr. LeFevre said.